Hormones 101
Written by Alia Brown, MD, FAAD as part of The Brown Skin Agenda Initiative.
Dermatologists and professionals know: if it’s happening in your body, it will show on your skin. It’s no surprise, then, that constantly fluctuating hormones can cause conditions that are unique to melanin-rich skin. Here, we’ll take a comprehensive A-to-Z dive into everything you’ve ever wanted to know about hormones and how they impact skin of color.
But first, what are hormones, and how do they impact skin health?
Hormones are chemicals that travel through your blood to your tissues, organs, muscles, and skin. They’re essential to everything from your metabolism to electrolyte balance and increased collagen production. They’re also very powerful: Just a little bit of hormonal imbalance in the body can set off a slew of systematic issues from poor sleep and stomach issues to skin issues like breakouts.
Do hormones affect skin of color differently?
In a word, yes. In skin of color where melanin production is already elevated, hormonal fluctuations can trigger an increase in melanin which ups the chances for hyperpigmentation. This hyperpigmentation can also be classified as melasma and can be triggered by things like oral contraceptives or pregnancy. Melanin-rich skin is also more susceptible to post-inflammatory hyperpigmentation (PIH), which is what happens when skin overproduces melanin at the site of a wound, scar, or injury – including acne. In the next few sections, we’ll go over the types of skin issues that may arise from hormonal imbalances, including hormonal acne, melasma, and acanthosis nigricans.
What is hormonal acne?
Hormonal acne is what happens when shifting hormones increase oil production in your skin. When that oil entangles with bacteria in the pores, the result is acne. Hormonal acne is mostly diagnosed in women, pregnant women, and menopausal women. Hormonal acne can be found on the face, neck, chest, shoulders, and back, and can be worsened by stress, humidity, and pollution.
While hormones like estrogen have been shown to help increase collagen production and hydration while bolstering a healthier skin barrier, estrogen imbalance can be the source of higher sensitivity before or during menstruation, as well as excessive oiliness and/or intensified dryness—both of which can create the ultimate breeding ground for breakouts and acne.
Acne may be a common skin concern (at one point or another, almost every human will experience it), but some research reveals that acne on darker skin tones is associated with inflammation and comedones, and darker skin tones are more susceptible to PIH and scarring. Treatment protocols for hormonal acne in dark skin must be mindful of a potential for irritation to prevent PIH from worsening.
What is melasma?
Melasma is the appearance of clusters or patches of dark spots that mostly appear on the cheeks, above the upper lip, and on the forehead. Melasma, like most hyperpigmentation, worsens in the summer when UV exposure is more common.
Research shows that melasma is more common in women and in people of color—further proving that melanin-rich skin tones are not immune to skin damage and must wear UV protection every single day. Pregnant women top the list, as their increased levels of estrogen and progesterone are believed to contribute to melasma, but melasma can also be induced by oral contraceptives or hormonal changes.
When considering a melasma treatment, some types of melasma do respond well. Epidermal melasma – or melasma on the outermost layer of the skin – is a bit easier to treat than dermal melasma – or melasma occurring in a deeper layer of the skin – due to its depth within the skin layers. Make sure to consult with your dermatologist to ensure you get the proper treatment, as some melasma treatments (like IPL lasers) are not safe for skin of color.
What is acanthosis nigricans?
Acanthosis nigricans is a skin condition that looks like hyperpigmented velvety patches or streaks. It commonly appears in skin folds, like the back of the neck, and can contribute to underarm darkness. While it’s mostly seen in patients with insulin issues/insulin resistance, people with hormonal disorders, such as Addison's disease, polycystic ovary syndrome (PCOS), or hypothyroidism can also develop acanthosis nigricans. While it can be visibly diagnosed, it may also require additional medical tests, as it may be an indicator of pre-diabetes or a thyroid condition. Research has not yet found a treatment for acanthosis nigricans, but if it is a condition induced by another medical condition like insulin resistance, it may fade on its own. Dermatologists may also prescribe retinoids/tretinoin cream, or recommend a laser, dermabrasion or chemical peels (like a VI Peel Body Treatment) to help lessen the intensity.
Are there any other skin conditions that are triggered by hormones?
It’s probable that science has only begun to scratch the surface on discovering the link between hormones and skin concerns, but progress is being made every single day.
As we already mentioned, patients with hormonal disorders, PCOS or hypothyroidism can develop hyperpigmented skin that’s diagnosed as acanthosis nigricans. And, excess facial hair can be an indication of hormone imbalance. This is the case with Hirsutism, a condition often triggered by an excess of hormones that causes excessive hair growth in women, in places where hair traditionally only grows on men (upper lip, lower abdomen, chest, and back). Hormone imbalances like PCOS, congenital adrenal hyperplasia, and Cushing syndrome (high levels of cortisol) are all known causes of Hirsutism.
Are there any effective treatments for balancing skin conditions caused by hormones?
Skin conditions triggered by hormones are some of the most challenging to treat, but dermatologists and medical professionals have an arsenal of tools at their disposal to help lessen the intensity—and those treatments go well beyond treating the face. Chemical peels, like the VI Peel, work by sloughing off the top layers of skin, and they’re powered by clinically proven ingredients that can help target melanocytes that are overproducing pigment. Your dermatologist or skincare expert may prescribe a series of VI Peel (for face) and VI Peel Body treatments to lessen the appearance of hormonal acne, melasma, and acanthosis nigricans.
Melanin-rich skin tones with hormonal acne and melasma may respond well to certain light-based lasers, like Aerolase. This laser penetrates deep within the sub-layers of the skin to vaporize acne-triggering bacteria and oils, while also encouraging collagen production that will push fresher, newer, plumper skin cells to the surface. There are some laser treatments that are not safe for skin of color, so make sure to speak to a licensed professional.
Retinoids, like retinols (available OTC) and retinoic acids (prescription only), remains the go-to gold standard for effectively treating hormonal acne. Retinoids stimulate cell turnover, helps de-clog pores, has anti-inflammatory properties, and even helps improve past acne scarring and dark marks. VI Derm Retinoic Serum with 0.1% Tretinoin (prescription only) is dermatologist-grade and fast-acting to help smooth out rough skin texture, diffuse dark spots, and encourage recovery from hormonal acne.
Although daily SPF use is important for maintaining healthy skin overall, SPF usage becomes especially crucial when undergoing the types of treatments listed above. Apply (and reapply every 2 hours) a broad-spectrum SPF of 30 or more, to ensure treatment progress is not delayed or even reversed. We like VI Derm SPF 50 Broad-Spectrum Sunscreen to help protect your skin during treatment.
Are there any treatments skin of color should avoid?
Chemical peeling options narrow for skin of color, as they can intensify or prolong hyperpigmentation. Avoid deep chemical peels and opt for skin-of color-safe corrective chemical peels, like a VI Peel. All VI Peels are safe and effective for darker skin. Laser can be an effective treatment for hormonal related skin issues, but there are some lasers that darker skin tones should stay away from, like IPL lasers. Lighter, non-ablative lasers like Aerolase is considered generally safe for all Fitzpatrick skin types. A dermatologist or medical professional can determine the best melasma treatment and treatments for hormonally induced conditions on skin of color, while assessing our skin’s responsivity before beginning treatment. No treatment should be considered or ruled out until you speak with a dermatologist or skincare professional.
Treating Hormonal Acne, Melasma, Acanthosis Nigricans, and more with VI Peel
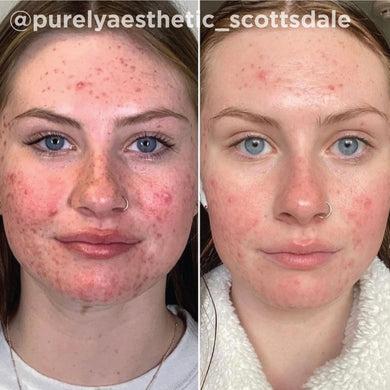
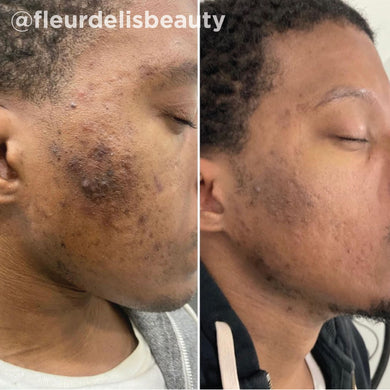
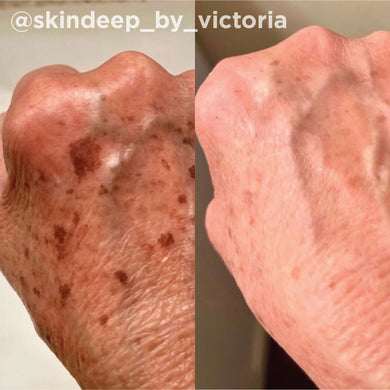
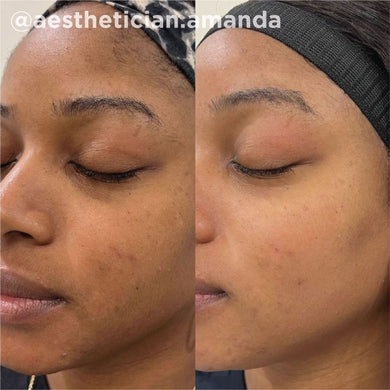
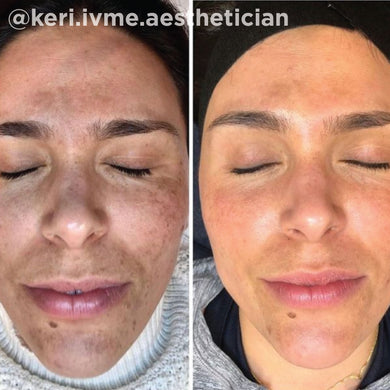
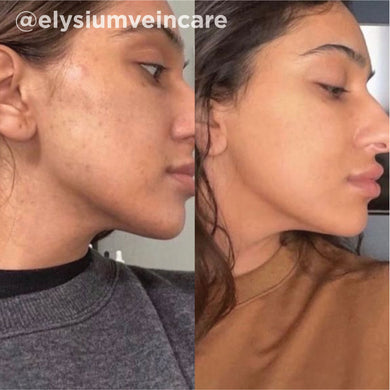
As a board-certified dermatologist for over 10 years, I’ve treated many skin issues triggered by hormonal imbalances. While these conditions can be frustrating for many, there are a host of treatments that are safe and effective for improving these conditions. I have found that the VI Peel treatment, both for the face and for body, has proved to be an exceptional treatment for many hormonal skin issues like hormonal acne, melasma, and acanthosis nigricans. The VI Peel treatment gently exfoliates and lifts stubborn pigment, improving the look of pigment related hormonal issues, like melasma and acanthosis nigricans. For pigment related issues, I’d recommend the VI Peel Precision Plus. VI Peels also fight hormonal acne breakouts, reducing the frequency and severity of the breakouts over time, and help lift the acne scarring that may come along with it. For hormonal acne and acne scarring, I recommend the VI Peel Purify with Precision Plus. Below are some photos of patients I’ve treated in the past, with great success.
Finally, no treatment beats taking preventative measures. Make sure to schedule your annual health screenings, as sometimes, we as practitioners can see subtle skin changes before the medical issue fully presents itself. Your healthcare practitioner or dermatologist can help. Cheers to glowing skin!



About Dr. Alia Brown, MD, FAAD
Dr. Alia Brown joined Georgia Dermatology Partners in 2010 after distinguishing herself at Meharry Medical College as an Honor’s Graduate and inductee into the Alpha Omega Alpha Medical Honor Society. She has published in multiple medical and dermatology journals. She is a member of the American Academy of Dermatology, American Medical Association, Women’s Dermatology Society, Alpha Omega Alpha Honor Medical Society, and Delta Sigma Theta Sorority Inc.
Dr. Brown specializes in partnering with patients to deliver the healthiest, most beautiful skin possible. As a highly skilled skin laser and surgery specialist, she focuses on cosmetic dermatology, including laser medicine and injectables. She places a high priority on her patients’ well-being and enjoys designing the most appropriate and successful treatment path for each individual. In addition, Dr. Brown enjoys traveling, exercising, and volunteer work with several civic organizations in her free time. Dr. Brown is married and has three children.
References:
The Journal of Clinical and Aesthetic Dermatology, 2010, volume 3, issue 4, pages 24-38
Journal of Cutaneous and Aesthetic Surgery, 2012, volume 5, issue 4, pages 247-253
Cleveland Clinic Website, Health & Diseases, Hormonal Acne
Cleveland Clinic Website, Health & Diseases, Melasma
Cedars Sinai Website, Health Library, Hirsutism in Women
The Mayo Clinic Website, Diseases and Conditions
American Academy of Dermatology Association Website, Diseases & Conditions